When developing your job safety analysis (JSA) or completing your Activity Hazard Analysis (AHA) Template (collectively “JSA” for the purposes of this article), it is important to understand the difference between face masks and respirators so that you can select the appropriate protection for the hazards identified in your JSA worksheet.
According to the Canadian Centre for Occupational Health and Safety, masks are designed to help prevent contamination of the work environment from large particles generated by the wearer. This helps to prevent the spread of the wearer’s spit or mucous. One example of this type of mask is a surgical mask; during surgical procedures, the mask helps protect the patient by preventing the wearers’ respiratory droplets from contacting the patient. Additionally, masks may be used to reduce the risk of body fluids, secretions, and excretions from reaching the wearer’s mouth and nose. Depending on the task, environment, and specific situation, both workers and the general public may find a benefit to wearing masks to help limit the spread of infections.
On the other hand, respirators are designed to reduce the wearer’s respiratory exposure to airborne contaminants such as particles, gases, and vapors. For the respirator to function as intended it must have a proper seal on the wearer’s face; without a proper seal, it will not provide proper protection. Respirators and filters must be selected based on the hazards present. The proper style and size need to be selected so that the respirator will properly fit the wearer’s face and provide a good seal.
In the US, respirators, such as the N95 respirators, are evaluated, tested and certified by the National Institute for Occupational Health and Safety (NIOSH) to meet set minimum performance requirements, whereas face masks are not subject to these same standards. The 'N95' designation means that when subjected to careful testing, the respirator blocks at least 95 percent of very small (0.3 micron) test particles. Many countries have their own standards for “N95” type respirators which may or may not meet the same NIOSH standards and may or may not supply the same level of protection.
The Centers for Disease Control and Prevention (CDC) does not recommend that the general public wear N95 respirators to protect themselves from respiratory diseases, including , but instead recommends that members of the public use simple cloth face coverings when in a public setting to slow the spread of the virus. The generally accepted reason for wearing masks is so that people who may have the virus and do not know they are infected will reduce the chances of transmitting the virus to others. In general, for this type of viral contaminant, under the current social gathering restrictions and social distancing protocols, the level of protection offered by an N95 mask is not thought to be necessary to protect the wearer. “I wear a mask to protect you; you wear a mask to protect me.” The US Food and Drug Administration (FDA) has additional details regarding masks and N95 respirators.
The U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC) has published guidance on how to get the most benefit from cloth and surgical masks by making sure the masks have a proper fit. CDC mask fit guidelines
It should be noted that most N95 respirators are manufactured for use in construction and other industrial type jobs that expose workers to dust and small particles. The manufacture of N95 respirators is regulated by the National Personal Protective Technology Laboratory (NPPTL), which is a division within NIOSH, and is part of the Centers for Disease Control and Prevention (CDC).
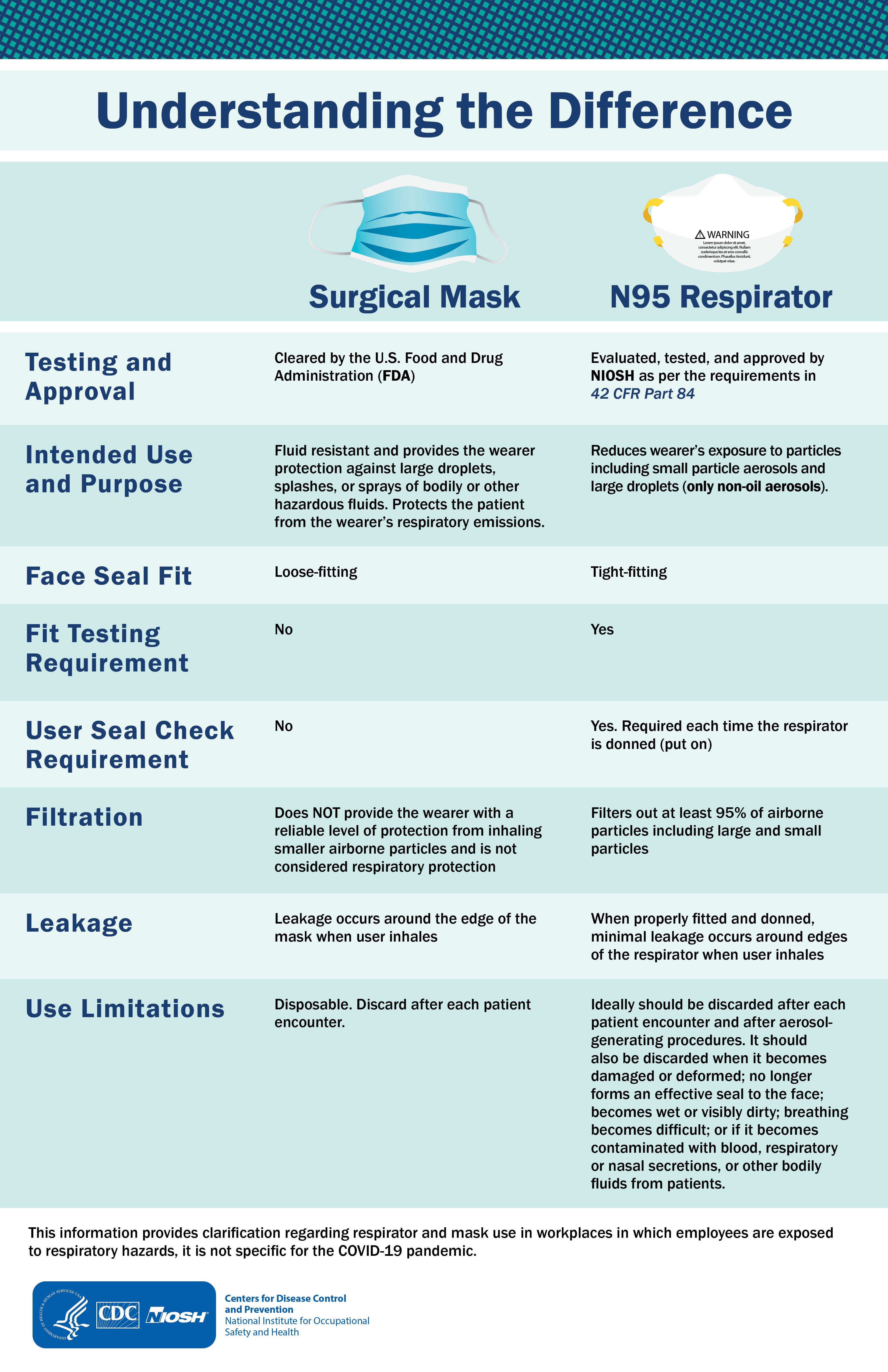
A summary of the differences between masks and respirators can be seen in the following graphic from the CDC and NIOSH.

As with all job-related hazards the best way to control a hazard is by eliminating it in the first place. Good JSA software will include ways to incorporate the standard hierarchy of controls into the job safety analysis. According to the CDC, controlling exposures to occupational hazards is a fundamental way to protect the public and medical personnel. Conventionally, a hierarchy has been used to achieve feasible and effective controls. Multiple control strategies can be implemented concurrently and or sequentially. This hierarchy can be represented as follows:
- Elimination
- Substitution
- Engineering controls
- Administrative controls
- Personal protective equipment (PPE)
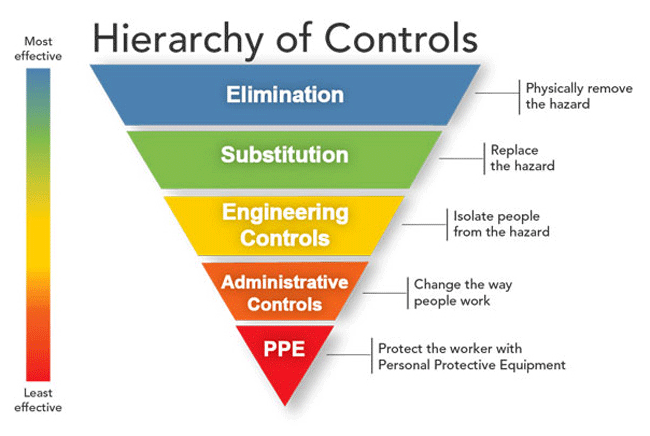
As can be seen, the use of personal protective equipment (PPE) is a final measure to protect people, not the first line of defense. Most health and safety professionals agree that to prevent infectious disease transmission, elimination (physically removing the hazard) and substitution (replacing the hazard) are not typically options for healthcare settings. However, exposures to transmissible respiratory pathogens can often be reduced or possibly avoided through engineering, administrative controls, and PPE.
For the public in their day to day interactions with other people, elimination or substitution might be more feasible, staying home (eliminating exposure to the hazard); avoiding contact with people outside the home (eliminating exposure to the hazard); work/school from home (substituting the former way of doing things for a new way which eliminates or reduces exposure to the hazard); etc.
In the healthcare setting, N95 respirators are the PPE most often used to control airborne exposures to infections, though their effectiveness is highly dependent upon proper fit and use. For the general public, surgical cloth and paper masks are the most commonly used PPE to mitigate exposure to airborne infections. The optimal way to prevent airborne transmission is to use a combination of interventions from across the hierarchy of controls, not just PPE alone. Applying a combination of controls can provide an additional degree of protection, even if one intervention fails or is not available.
Respirators, when required to protect health care workers from airborne contaminants such as some infectious agents, must be used in the context of a comprehensive, written respiratory protection program that meets the requirements of OSHA’s Respiratory Protection standard external icon. Your Activity Hazard Analysis and related program should include medical evaluations, training, and fit testing.
JSABuilder.com is an ideal on-line job safety analysis app to assist in evaluating the hazards and minimizing risks to your workers and the general public.